In our last blog, we discussed variables in CPAP Therapy that can contribute to a better night’s sleep. Because there are endless combinations when you consider the various types of CPAP machines, masks, pressure settings, humidification levels and other settings, as well as the care and training you receive from your CPAP Supplier. We will answer the following questions in this blog:
- What are the five types of positive air pressure (PAP) therapy machines and what is the right machine for you?
- How can CPAP therapy be modified to treat patients with mild to severe OSA symptoms?
- How imperative is finding a sleep specialist or a physician well-versed in sleep medicine to the success of your accurate diagnosis and effective treatment?
Five Types of PAP Machines and their Functionality Differences
Let’s first talk about the commonalities between the five machines. All five types of CPAP machines are all forms of positive airway pressure therapy (PAP), and utilize a mask and tubing to provide a gentle flow of pressurized, filtered air to keep your airway open. All PAP therapy machines focus on keeping obstructions from blocking your ability to breathe when you’re asleep. What are the differences?

- CPAP: CPAP stands for “continuous positive airway pressure” because provide a single, fixed air pressure to the patient’s airway. The pressure is determined by your physician or sleep specialist’s prescription, which is between 4 cm of water pressure and 20 cm of water pressure.
- APAP or AutoPap: AutoPap machines deliver auto-titrating, or auto-adjusting, air pressure depending on the patient’s needs. The range of pressure is set by your physician or sleep specialist’s prescription. If the patient tosses and turns or moves through the various stages of sleep, the machine will sense that the breathing pattern has changed and increase or decrease the airflow to keep the airway open.
- BiPAP or Bilevel: While CPAP and Autopap use a single air pressure, BiPAP use two – one pressure setting for inhalation and another for exhalation. For those with more severe OSA or for patients with more frequent apnea events (where they stop breathing), the dual pressure provides a more natural breathing experience and a better night’s sleep. *This has also proven helpful for those with severe respiratory illnesses due to COVID-19.
- ASV: Adaptive Servo Ventilation (ASV) is a non-invasive ventilatory treatment that continuously monitors and adjust to correct the patient’s breathing problem. ASV’s pressure target is not a fixed value but adjusts according to input from the patient and adapts to the patient’s breathing patterns. Comfort of PAP therapy increases as the subtle machine’s pressure changes according to the patient’s needs.
- BiLevel with Backup Rate: Similar to BiPAP or Bilevel, but the device triggers to IPAP (Inspiratory positive airway pressure) on patient inspiratory effort. The backup rate is a spontaneous or timed mode that is set to ensure that patients still receive a minimum number of breaths per minute if they fail to breathe spontaneously. The backup rate can be set at automatic or can be set manually, which is determined by the patient’s physician’s prescription.
Another Variable is Pressure Settings of your CPAP Machine
While Autopap varies the settings automatically according to the patient’s needs, other machines are set according to your physician or sleep specialists.
CPAP pressure is measured in centimeters of water (cmH2O)—a special unit of measurement that measures water pressure. This unit measures how much pressure a column of water exerts against its container. The settings of water pressure (abbreviated as cm of H2O or CWP) vary from 4cm to 20cm, with an average of 10cm.
The pressure settings are based on the AHI (apnea-hypopnea index) which is scored on how many times you stop breathing over the course of an hour of sleep. Based on the AHI, the severity of OSA is classified as follows:
- None/Minimal: AHI of 0 to 5 per hour
- Mild: AHI of 5 to 15 per hour
- Moderate: AHI of 15 to 30
- Severe: AHI of over 30
If your pressure is too high:
- the patient will feel discomfort in mouth, nose and airways,
- a burning sensation in the nose and throat,
- hearing issues from fluid entering the ears at night,
- aerophagia (where the patient is gasping for air during the night) and thus swallow air into their stomachs, which can cause bloating, gas, discomfort and excessive belching,
- and daytime fatigue, as the incorrect air pressure setting is defeating the purpose of the CPAP therapy.
If your pressure is too low:
- the patient will have five or more apnea or hypopnea events per hour;
- feeling air-starved during the night,
- persistent snoring,
- aerophagia, (see description above)
- and daytime fatigue due to a poor night’s sleep.
If any of these symptoms are occurring, make sure to call your physician so they can adjust your settings. It is not out of the ordinary to make adjustments, especially in the beginning stages of using CPAP, so be patient and understand that there are many adjustments that can be made if you’re initially experiencing discomfort or not achieving a substantial improvement in your sleep quality.
Other variables include:
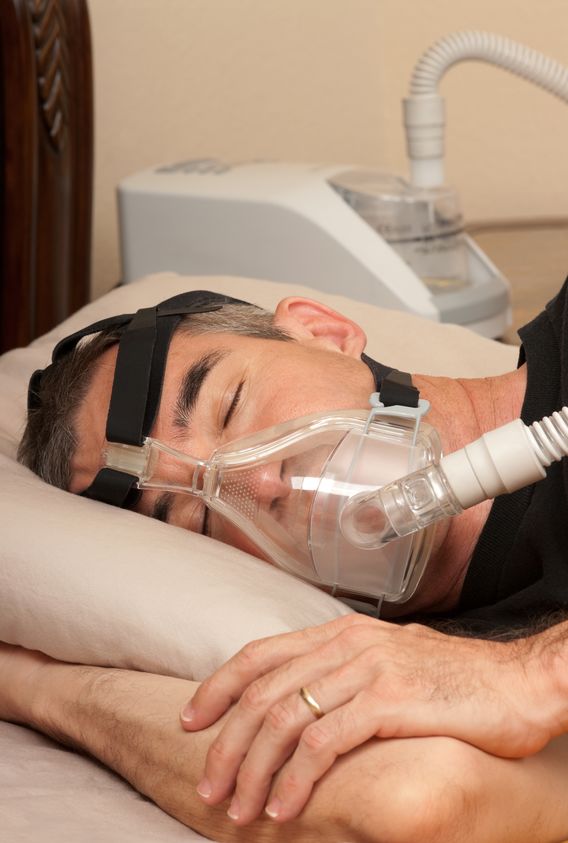
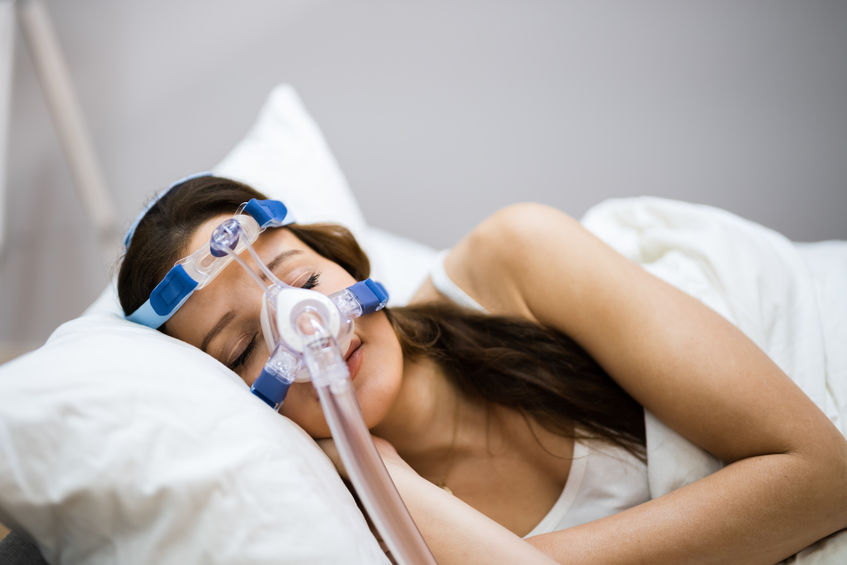
Mask Types: There are three types of mask: full face masks, nasal masks and nasal pillow masks. Within each manufacturer, there are variations in each of these three types so the possibilities are widely varied for male, female, and pediatric patients. (See our previous blog “Which Type of CPAP Mask is Best for Me?”).
Ramp Settings: The Ramp Time is used to designate the amount of time it will take to ramp to a set pressure. Usually set from 15 to 30 minutes, it allows the pressure to gradually increase to prescribed pressures for the comfort of the patient as they fall asleep. The ramp time can reset each time the patient awakes through the night.
EPR Settings: Expiratory pressure relief (EPR™) maintains the optimal treatment for the patient during inhalation and reduces pressure during exhalation. If your CPAP machine as an AutoSet Response comfort setting, it can offer gentler pressure increases and a smoother night’s sleep to help patients with high pressure intolerance.
C-FLEX Feature: C-Flex is available on some automatic CPAP machines and will lower the pressure when you exhale and slowly increase the pressure when you inhale. The C-Flex feature essentially breathes along with you while you sleep.
Humidification Levels: The CPAP humidifier adds moisture to your therapy air. To prevent dry mouth or dry nose discomfort, the patient can add humidity to the therapy air when using your CPAP machine. The DME professional (CPAP Supplier) can either set the humidification levels or teach the patient to do this, unless the physician has previously prescribed set levels for the patient.
Signs that the humidification levels need to be adjusted are:
- burning or dryness of nasal passage,
- runny or stuffy nose,
- dry mouth,
- sneezing during CPAP treatment,
- sore or dry throat,
- nosebleeds,
If your chamber empties of water before morning or is collecting a residue that appears to be mold, you may need to talk to your DME provider to adjust settings. Make sure you are only using distilled water in your humidifier and changing the water out each night.
Heated Tubing: Heated tubing maintains the warm temperature of the air as it travels from the humidifier’s water chamber up to the mask. Using heated tubing can counter irritation and dryness in even the most sensitive patients. The heated tubing prevents condensation buildup in the tube, which prevents ‘rainout’ (when the heated air cools in your tubing thus reaching your mask as water rather than humidification, thus causing the patient to get a damp face). Rainout can disrupt the patients sleep by waking them from the discomfort of a wet face as well as hearing the annoying gurgling sound in the tube from excess condensation.

“Patients over 60 years of age are five times more likely to require humidification.” – Sleepapnea.org
Heated tubing would also be recommended for patients on certain medications, those with chronic mucosal disease, and those who have had UPPP surgery, as well as those who live in drier, colder climates. Although even in humid climates, CPAP can still cause dryness so here at Everything CPAP, we find the benefits of heated tubing outweigh the non-heated, so we usually recommend them to most of our patients.
CPAP Smell: Some patients might find the smell of the water vapors a deterrent, so we recommend using aromatherapy for those sensitive to the smell. Do not put any oils or fragrance in the water chamber as this can cause serious health hazards. If used properly, essential oils and aromatics can compliment your CPAP therapy. We recommend the Pur-sleep CPAP Aromatherapy Starter Kit.
How to use: Pur-Sleep’s Passive Diffusion System uses a Raised Tray and Reusable Diffuser Wafers, made of a specially compressed fiber material, to lightly scent the air drawn into your CPAP to promote a more conducive sleep environment. With Pur-Sleep you simply place a few drops of Essential Oil on a Diffuser Pad and then position it in front of your CPAP/BiPAP filter; after that, start your sleep therapy as usual.
The Last Variable, but the Most Important – Find a Sleep Specialists that Understands the Diagnosis and Treatment of OSA
There are over 8,000 sleep specialists in the United States, but many primary care doctors and physicians can also diagnose and treat your sleep disorder symptoms. A Sleep Specialist is a doctor who diagnoses and treats sleep disorders. Most sleep specialists train in internal medicine, psychiatry, pediatrics, or neurology during residency. After completing residency, they complete a fellowship program in sleep medicine. Doctors who receive training in sleep medicine get their board certification from the American Board of Sleep Medicine, which is part of the American Board of Medical Specialties. A sleep specialist can diagnose and treat sleep disorders, such as OSA, restless legs syndrome (RLS), or insomnia.

While your primary care doctor can assess the situation, they would more than likely refer you a sleep specialist for evaluation for proper diagnosis and treatment, as well as maintenance of the above named variables to ensure you are getting the most effective treatment from your CPAP therapy.
Where can you find a sleep specialist: Most major hospitals have sleep labs and there are usually specialized sleep centers in most major metropolitan areas. For the Boise, Idaho and Treasure Valley area, we have the following:
Feel free to call our staff to get started on your CPAP journey, as well as recommendations for sleep specialists in your area and how to fit, setup and use your CPAP machine, mask and tubing according to your doctor’s prescription.
We are here to help! The owners and employees of Everything CPAP are dedicated to the improvement and extension of our patient’s lives through personalized care, use of state-of-the-art equipment, constant innovation, and clinical research. Our process has proven success as our patients’ adherence rates are over 86%.
Home Test or Lab Test? – That is the Question
Our next blog will discuss the process of taking a home sleep test versus a lab sleep test, the pros and cons of each and how in the time of COVID-19, each has been affected.





