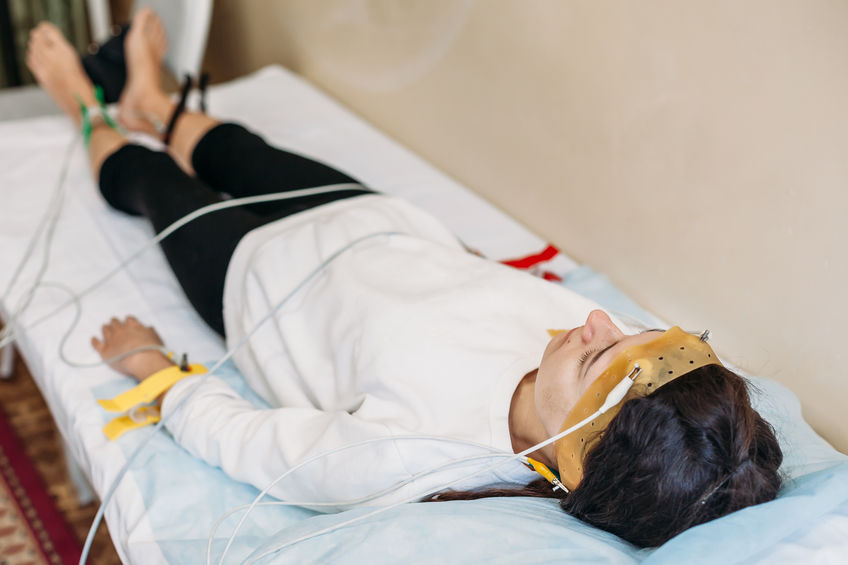
What is Polysomnography?
Polysomnography, also called a sleep study, is a comprehensive test used to diagnose sleep disorders by monitoring and recording: your brain waves, the oxygen level in your blood, heart rate and breathing, as well as eye and leg movements during the study.
The Sleep Study can be done at a hospital, a sleep center, or at the patient’s home, and is usually performed at night, with some exceptions for shift workers who typically sleep during the day. In addition to diagnosing sleep disorders, including obstructive sleep apnea (OSA), the polysomnography provides data to determine the CPAP Therapy variables (type of CPAP machine, pressure settings, Ramp settings, humidification levels, and tubing types) specific to the patient’s needs.
*See our last blog for a detailed explanation of these variables: ‘A Personalized Approach to your CPAP Therapy’
In this article, we will define the four types of Sleep Studies, what they monitor, where they can be performed, and why physicians order them, as well insurance considerations for each. Also, we will discuss the pros and cons of home sleep tests versus one that takes place in a sleep center or hospital. Also, in the time of Covid-19, home sleep tests have trended upward based on CDC guidelines and how this has impacted the future of polysomnography.
The Four Types of Polysomnography (PSG)
“35% of adults are not getting the recommended 7 hours of sleep each night. More than a third of American adults are not getting enough sleep on a regular basis, according to a 2016 study in the Centers for Disease Control and Prevention’s (CDC) Morbidity and Mortality Weekly Report.”
– CDC.gov
Since a good night’s sleep is critical to good health, it’s imperative to determine if poor sleep is based on poor sleep hygiene or from an undiagnosed sleep disorder. That is where Polysomnography comes in. The CDC suggests that healthcare providers routinely assess their patients’ sleep patterns and discuss sleep-related problems such as snoring and excessive daytime sleepiness, as part of their regular checkups. Why?
For our bodies and minds to function properly, a consistent pattern of seven hours of quality sleep each night is required. If the healthcare physician or the patient suspect the lack of quality sleep is based on a sleep disorder then the next step is a sleep study to provide accurate diagnosis. Which type and why?

TYPE I POLYSOMNOGRAPHY
- Where it is performed: Type 1 is an overnight technician-attended Sleep Study that takes place in a Sleep Laboratory facility or hospital. The American Thoracic Society and the American Academy of Sleep Medicine have recommended supervised PSG in the sleep laboratory over two nights for the diagnosis of OSA and the initiation of CPAP therapy.
- Why ordered: It is used to help determine the cause of excessive daytime sleepiness as well as diagnose various sleep disorders.
- What is monitored: Type 1 studies brain waves, heartbeats, breathing, as well as eye movements, limb movements and oxygen in patient’s blood. An attended facility-based polysomnogram is a comprehensive diagnostic sleep test that includes: electroencephalography (EEG), electro-oculography (EOG), electromyography (EMG), heart rate or electrocardiography (ECG), airflow, breathing/respiratory effort, and arterial oxygen saturation (SaO2). Type I studies are usually performed in a sleep laboratory facility where a technologist supervises the recording during sleep time and has the ability to intervene if needed.
- Insurance Considerations: Type 1 PSG is covered when used to aid the diagnosis of OSA in beneficiaries who have clinical signs and symptoms of OSA is performed in a sleep lab facility.
TYPE II POLYSOMNOGRAPY
- Where it is performed: Type II utilizes monitoring devices that can be performed outside of the laboratory. The major difference from Type 1 is that the technologist may not be present and the test can be monitored by comprehensive portable devices. Type II is the most advanced sleep testing device but is not used too often because of the need to monitor EEG. Therefore, the Type II can also be completed at the patient’s home, as well as in a sleep lab or hospital.
- Why ordered: Type II is ordered to aid in the diagnosis of OSA or if the patient and/or the physician is unsure of the cause of poor sleep, because a Type II can provide additional information to help uncover the root cause.
- What is monitored: Type II monitors a minimum of seven channels (EEG, EOG, EMG, ECG-heart rate, airflow, breathing/respiratory effort, Sa02) and this type of device also monitors sleep staging, so AHI can be calculated. In addition to monitoring your breathing activity, oxygen levels, and heart rate, a level 2 sleep study monitors brain and muscle activity.
- Insurance Considerations: Type II sleep testing devices are covered when used to aid the diagnosis of OSA in beneficiaries who have clinical signs and symptoms indicative of OSA if performed in or out of the sleep lab facility or attended in a sleep lab facility
TYPE III POLYSOMNOGRAPY
- Where it is performed: Type III are often referred to a home sleep apnea test (HSAT) and it’s performed in the comfort of your home, not in a sleep lab or hospital. The patient is provided with a sleep study kit that records breathing activity, oxygen levels and heartrate through the course of the night.
- Why ordered: Type III is best suited for patients who suspect they are at risk of sleep apnea only and is often prescribed for patients who lack the need to monitor EEG.
- What is monitored: Type III monitors have a minimum of four monitored channels including ventilation and airflow (at least two channels of respiratory movement and/or airflow), heart rate or ECG, and arterial oxygen saturation. Some devices may also record snoring, detect light or a means to determine body position.
- Insurance Considerations: Type III sleep testing devices are covered when used to aid the diagnosis of OSA in beneficiaries who have clinical signs and symptoms indicative of OSA if performed in or out of the sleep lab facility or attended in a sleep lab facility.
TYPE IV POLYSOMNOGRAPY

- Where it is performed: Type IV devices are called continuous single or dual bioparameter devices, that record one or two variables (arterial oxygen saturation and airflow) and can be used with or without a technician, thus it can be performed at a sleep lab facility, at a hospital or at the patient’s home. Type IV are usually performed at home.
- Why ordered: Type IV may often be used to test for Pediatric Sleep disorders, although home sleep tests are not approved for patients under the age of 18, thus regardless of type, pediatric patients are required to perform the sleep study in the lab. Because Medicare and many insurance types require at least three channels, most current home sleep testing devices ordered are Type III. *Type IV devices are not often prescribed.
- What is monitored: Type IV devices measures three or more channels, that include actigraphy, oximetry and peripheral arterial tone, and may measure one, two, three or more parameters but do not meet the criteria of a higher category devices.
- Insurance Considerations: Type IV devices are covered when measuring three or more channels, one of which is airflow, and used to aid the diagnosis of OSA in beneficiaries who have signs and symptoms indicative of OSA if performed in or out of the sleep lab facility or attended in a sleep lab facility.
The Pros and Cons of Home Sleep Testing
“If you are being told that you snore, snort and gasp, if you have disrupted sleep or are sleepy during the day, and you are overweight or obese, an at-home sleep apnea test may be very appropriate. Talk with your clinical provider about your options.”
– Susheel P. Patil, MD, PhD, clinical director of the Johns Hopkins Sleep Medicine Program
How Home Sleep Tests Work
After a doctor or sleep physician prescribes it, the patient receives the sleep study kit with instruction and training conducted by a sleep professional. After testing with reusable units, the device is returned for the data to be downloaded and evaluated, and a sleep physician then provides a report. The equipment is then conditioned to send to the next patient. After completion of the test, your results are securely uploaded to the cloud. A board-certified sleep physician will interpret the results, and if necessary, will recommend treatment and provide a prescription.
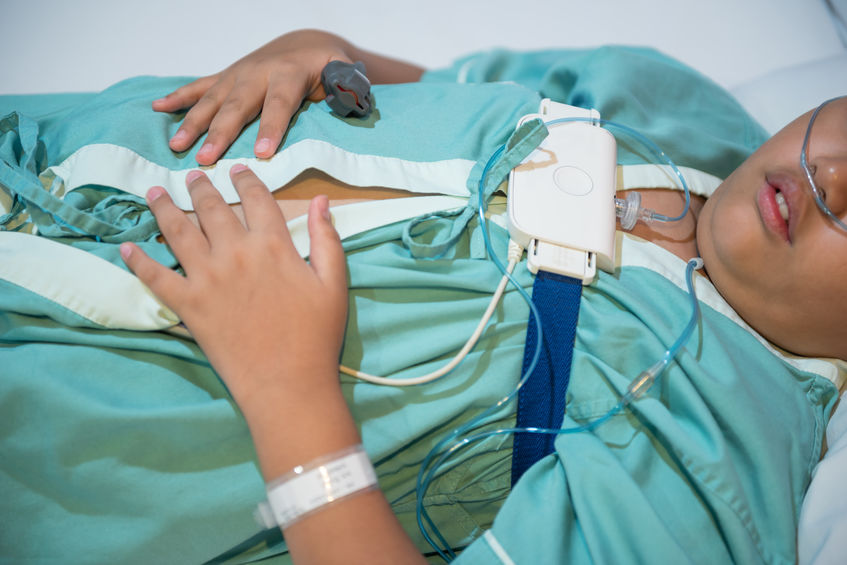
Less Sensors = More Comfort & Less Accuracy
Sensors are placed on the patient’s finger to measure oxygen levels, a nasal cannula is inserted in the patient’s nostrils and secured around the ears, and other sensors are placed on the abdomen and chest to measure the rise and fall as they breathe. Compared to an in-lab test: Home test have three monitoring sensors, rather than 15-20+ sensors on the head and chest in a lab sleep test. While this can make it more comfortable for the patient, it also means a decrease in variables monitored which can decrease accuracy of diagnosis. Because of limited variables measured, a home sleep test is only meant to evaluate a patient for sleep apnea, as it monitors breathing patters exclusively, and not the quality of the sleep itself. For example, a home test will not measure how long the patient is in a light or deep sleep and not all sleep disorders are caused by breathing trouble, for example: narcolepsy. If the patient’s symptoms persist, they may need to repeat the sleep study in a sleep laboratory facility.
Less Time & Less Expensive
Home sleep testing is usually completed in one to two nights unless the sleep test readings were incomplete if the patient did not sleep well or for an adequate amount of time. Because it is unattended, with just three variables monitored, and is completed in one night, home sleep tests are less expensive. Because the cost is usually a third to a fifth of the cost of in-lab study, they are typically covered by insurance. Because of the cost-savings for insurance companies, home tests have become increasingly popular in the last five years.
In the Comfort of your Home & Bed
Home sleep testing are completed in the comfort of the patient’s home, which can mean a more accurate reading because the patient slept better in their own bed. On the other hand, many sleep lab facilities have designed their lab rooms for increased comfort, similar to hotel rooms. By doing so, this can help reduce patient anxiety and help to counter the “First Night Effect”, since some patients may not sleep well the first night and may need a second night in the lab. Your sleep specialist will understand that the First Night Effect is possibility and will take into consideration when interpreting results.
Further Study May be Needed
Regardless, if you had a home sleep test or an in-lab test, you may be required to visit the lab for a titration study within a set time after diagnosis of the initial sleep study. A CPAP titration study is a type of in-lab sleep study used to titrate continuous positive airway pressure (CPAP) therapy. CPAP is a common treatment used to manage sleep-related breathing disorders including obstructive sleep apnea, central sleep apnea, hypoventilation, and hypoxemia.
Sleep Studies in the Time of Covid

In the last year, patients using home sleep tests have increased during the pandemic, to keep the staff and the patients safe because sleep testing at home allows the patient to avoid entering potentially infectious spaces. If you are required to visit a lab for your sleep test, a negative Covid test is often required. Some labs
may have you test negative three days before the sleep study. Others may use a rapid test the day of the study.
However, with the convenience of telehealth appointments and virtual meetings, Everything CPAP can train you on how to fit your mask, set up your machine, clean your CPAP equipment and adjust your settings accordingly without leaving your home. Everything CPAP offers ongoing support for refitting, product or part replacement, order refills on accessories, and are accessible for any of your questions and address any of your concerns, day or night.
At Everything CPAP, if you need technical support after hours, our staff is available to our existing patients twenty-four hours a day, seven days a week to prevent or address treatment failures. Your comfort and success are our priority so that is why Everything CPAP offers an unconditional Mask Fit Guarantee with over 200 mask options, proper fitting by our staff at our initial visit as well as ongoing support for our patients.
Do you suspect you are dealing with a sleep disorder?